Helping Healthcare Providers Grow Their Revenue, Improve Engagement, and Provide Quality Care
Our data-driven technology solutions give you the tools and resources needed to reach your full potential.
Helping Healthcare Providers Grow Their Revenue, Improve Engagement, And Provide Quality Care
Our data-driven technology solutions give you the tools and resources needed to reach your full potential.
Announcing Our Brand New Product
Cancellation Prediction™
Our New Tool Leverages AI and Machine Learning Technologies to Give You the Power to Predict and Prevent Cancellations
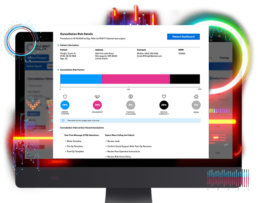
Cancellation Prediction™
Our New Tool Leverages AI and Machine Learning Technologies to Give You the Power to Predict and Prevent Cancellations


Harnessing the Power of Patient Data
Our proprietary technology leverages millions of data points in order to provide you with intelligent tools that improve operational efficiency, maximize engagement, boost revenue, and enable you to deliver personalized care experiences that result in more satisfied patients.

Harnessing the Power of Patient Data
Our proprietary technology leverages millions of data points in order to provide you with intelligent tools that improve operational efficiency, maximize engagement, boost revenue, and enable you to deliver personalized care experiences that result in more satisfied patients.
We Believe Every Patient Deserves a Helpful, Transparent, Easy to Navigate Healthcare Experience
We provide the most effective, affordable, and patient-friendly solutions that produce excellent customer satisfaction.

We Believe Every Patient Deserves a Helpful, Transparent, Easy to Navigate Healthcare Experience
We provide the most effective, affordable, and patient-friendly solutions that produce excellent customer satisfaction.

Assisting Providers Nationwide
2,000+
Clients we work with
20M
Patients represented
$3B
in managed balances
49
states we're operating in
Who We Serve
ASCs
Hospitals
Physician Groups
Anesthesia
Imaging
Patients

How Our Solutions Benefit You
View High-Risk Patient Alerts
Improve Patient Engagement
Drive More Cases to Your Facility
Save Staff Time
Increase Cash Flow
Enhance Patient Satisfaction
Reduce Cancellations
Boost Operational Efficiency
Maximize Patient Safety
Ready to Experience a Personalized Demo?
Please fill out your contact information below to speak with an expert.
Looking For Help?
Whether you are a patient needing support, looking for answers to frequently asked questions, or needing to contact us,
please choose the option that best fits your needs below.
Frequently Asked Questions
Find answers to common questions about our services or policies.